People in their 70s vividly remember a disease that frightened people as much as AIDS, or for many, COVID, frightens people today. A child who had been chasing friends around a piñata found themselves counting ceiling tiles in isolation, without enough strength to walk, the next day. Parents feared their children would be the next victim of the disease that claimed thousands of young lives and debilitated hundreds of thousands.
The first major documented U.S. outbreak of poliomyelitis, or polio for short, occurred in 1894 in Vermont, killing 18 people and permanently paralyzing 132. Its contagious properties were not identified until 1905 after a polio outbreak in Sweden, where it was discovered the virus could be transferred from person to person.
In the early 1950s, polio became a major concern. According to the CDC, 57,628 polio cases were reported in the United States in 1952, more than 21,000 of them paralytic cases. Ted Quick was 7 years old in 1953, living a simple life in Minden, Nebraska, when he was diagnosed with polio after attending a friend’s birthday party.
“I have a brother whose birthday is September 25,” Quick said. “On the 22nd, my dad had bought a [toy] tractor that we needed to put together, so we put it together that night and I rode it all over the house. The next day, I woke up and I was kind of stiff and sore, and I thought it was strange. When I got up to go to the bathroom that night I fell down twice. My mother heard me fall and got up to help me to the bathroom. When I laid back down in bed she said, ‘that’s OK you’re just tired.’ I just had to smile at her because I knew I had polio and Mom didn’t want to scare me.”
When Quick woke up the next morning, he was unable to get out of bed and was rushed to the doctor in town, who immediately called Children’s Memorial Hospital in Omaha to prepare them for Quick’s arrival. His parents jumped into action, and his father’s lead foot caused a brief setback during the three-hour trek to Omaha.
After explaining the situation, the officer escorted them, lights on and sirens blaring, to the hospital. Quick, and thousands of others, were subjected to painful procedures by medical professionals. Shots in the leg multiple times a day, grueling physical therapy, and isolation became a reality for polio victims in the United States.
Chip Mackenzie was a first-grade student in California when he was diagnosed with polio in March 1952.
“I remember the isolation of the first week or so at Sacramento County Hospital and the horrible tasting medicine—they had to hold my jaw open and pour [it] down my throat,” Mackenzie said. “I was moved to Sutter Hospital, where I started physical therapy to prevent my muscles from tightening up. It was painful. After three months there, I was moved to San Francisco Children’s Hospital, where the therapy continued and resulted in my being able to walk with long leg braces and crutches.”
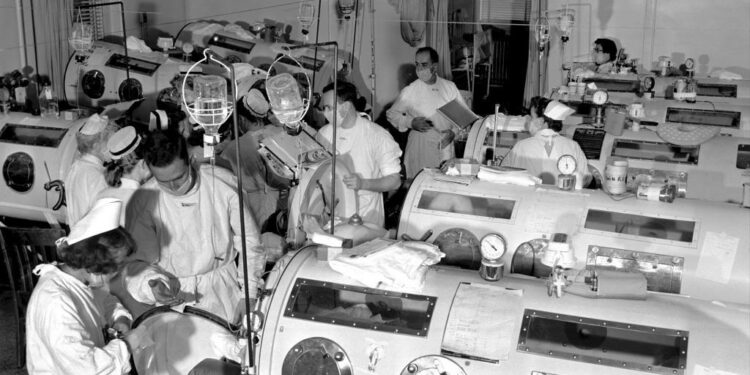
For the unluckiest of patients, polio would begin in their extremities and eventually move to the lungs, and many were unable to breathe when the virus paralyzed muscle groups in the chest. These children were placed in an iron lung that assisted their breathing until they were well enough to breathe on their own. At the height of the polio epidemic, a reported 1,200 Americans relied on an iron lung to stay alive. NPR reported in October 2021 that Martha Lillard, who lives in Oklahoma, still uses an iron lung at night; the New York Post reported in early November 2021 that Paul Alexander, 75, lives in Texas and is the last person confined to an iron lung.
Early treatments for paralyzed muscles advocated the use of splints to prevent muscle tightening and rest for the affected muscles. Many paralyzed polio patients laid in plaster body casts for months. Those long periods in a cast often resulted in atrophy of affected and healthy muscles.
The epidemic spurred research for a vaccine that had begun in the 1930s by Franklin D. Roosevelt, himself afflicted with polio, who created the National Foundation for Infantile Paralysis, which was quickly renamed the March of Dimes after its national campaign. Following Roosevelt’s death in 1946, the U.S. treasury began to print Franklin’s profile on dimes in honor of his support of the March of Dimes.
With help from funds garnered through the March of Dimes, Dr. Jonas Salk created a polio vaccine that began distribution in 1955, and in 1962, an oral vaccine developed by Dr. Albert Sabin began to be used. Following the mass vaccination of children in the mid-1950s, 2,525 cases were reported in 1960 and 61 cases in 1965. Polio was declared eradicated in the United States in 1979.
“Future generations don’t even know what polio was like,” Mackenzie said. “I ran into several people in the 2010s who indicated I was the first polio person they had ever met.”
Although polio has been eradicated for over 40 years in the U.S., victims are still carrying the heavy burdens their disease left behind. Some found it helpful to speak about their experiences with others who have been through similar struggles.
The Nebraska Polio Survivors Association was created in 1984 by a survivor who wanted to spread awareness about polio and post-polio syndrome. The first newsletter, printed in April 1985, said the coordinator had heard from more than 450 survivors interested in becoming a member. Support groups were set up throughout the state so those affected could receive support. Any polio survivor, family member, or member of the medical community are welcome to attend meetings or receive the organization’s quarterly newsletter.
“I believe NPSA is an important resource to respond to polio survivors’ needs for information on polio and post-polio syndrome through group meetings, educational programming, and our newsletters,” executive director Elaine Allen said. “In addition, part of our mission is to educate the public and the health care community concerning polio and post-polio syndrome. It’s important for polio survivors to understand that many times, they have to educate their health care providers about PPS because it is not a condition that is taught in most medical schools.”
Visit polioplace.org to learn more about polio and the NPSA.
This article originally appeared in the January 2022 issue of Omaha Magazine. To receive the magazine, click here to subscribe.










![[L to R] Daisy Hutzell-Rodman, Julius Fredrick, Kim Carpenter.](https://www.omahamagazine.com/wp-content/uploads/sites/2/2024/04/BTL-350x250.png)

